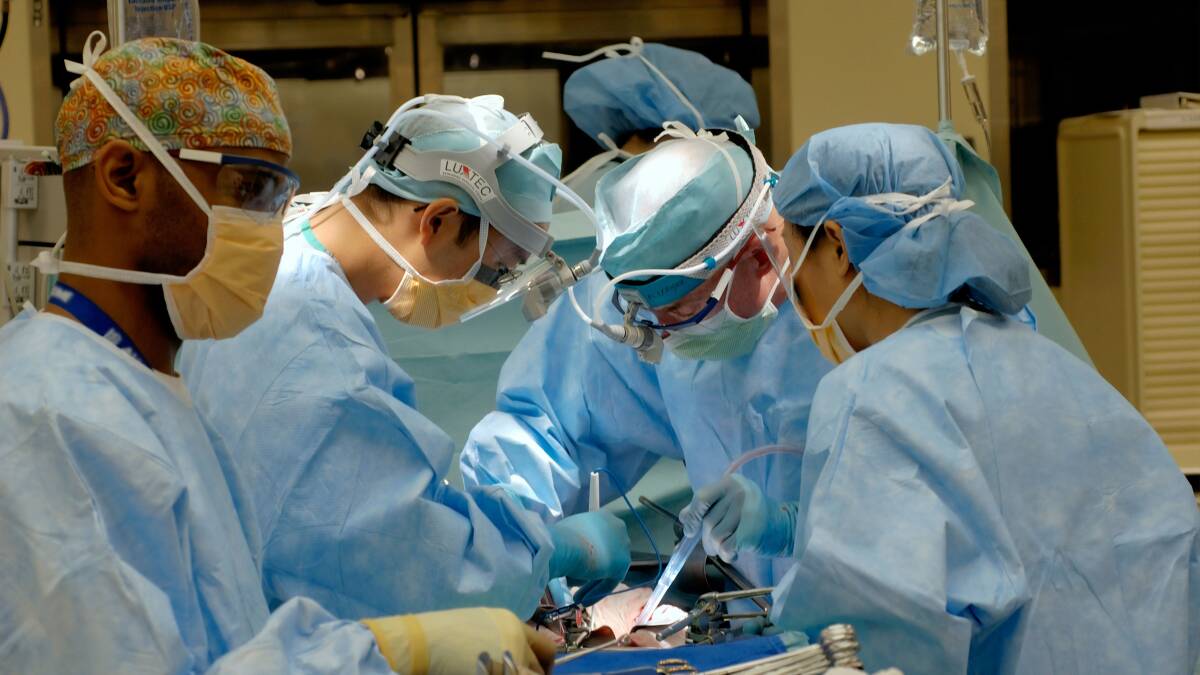
The use of heart-lung machines during heart surgery is common, but up to half of surgery patients subsequently report delirium, short term memory loss, emotional disturbance, trouble concentrating or problem solving.
Create a free account to read this article
$0/
(min cost $0)
or signup to continue reading
And 1.2-1.6 per cent of patients develop stroke following their surgeries. Up until now, the reason for this has been unclear.
However, researchers at The Florey are one step closer to finding new treatments to prevent brain injuries after discovering the problem is the result of inflammation in the brain caused by the heart-lung machine, which is used to take over the workload of the heart and lungs during surgery, diverting blood and oxygen around the body.
The Florey's research, published in Anesthesia & Analgesia, shows world-first evidence of heart-lung machines causing inflammation in the brain and - as a result - brain injuries in patients afterwards.
It also shows why this is happening, paving the way for preventative treatments.
Lead researcher Associate Professor Yugeesh Lankadeva, said the findings will reduce the short-term risk of in-hospital death and improve the long-term quality of life for patients following heart surgery.
"When a patient has a heart transplant, a heart bypass or any procedures to repair or replace heart valves, the heart-lung machine is vital for cardiac surgeons to carry out these major operations. So, it's important to understand how the brain was being impacted," Associate Professor Lankadeva said.
The researcher found neurological complications are likely occurring due to a profound inflammatory response caused by the blood passing through the heart-lung machine.
"As it (blood) passes through the synthetic tubing and enters the body, inflammatory mediators are released within the bloodstream. This is known as a 'systemic inflammatory response' which causes neuroinflammation in several key regions of the brain," Associate Professor Lankadeva said.
Researchers saw the systemic inflammatory response was fast and was likely to be causing neuroinflammation by disrupting the blood-brain barrier, the biological wall that protects the brain.
Importantly, this research also disproves a theory that a lack of oxygen in the brain during surgery is the cause of acute brain injury. Instead, the team found that neuroinflammatory injury occurs even in the absence of reduced oxygen levels - also known as hypoxia - in the brain.
"Thanks to our research we know why these neurological complications occur and when to administer treatment for the best chance of success," Associate Professor Lankadeva said.
"The missing piece now is the treatment itself. That is our next step - to develop targeted therapies that prevent neuroinflammation from occurring, stopping injury to the brain before it happens."

