Australian researchers are seeking volunteers aged 40 and over living with severe emphysema and collateral ventilation for a study of a new treatment.
The study, named COVE, involves a novel approach where two treatments are used together to help address the issue. Currently, people who have severe emphysema and collateral ventilation have limited options to treatment due to the nature of the conditions.
This new approach will be the first time it's done in humans.
According to an article in Medical Journal of Australia's (MJAs) InSight+, authored by COVE Study Lead Investigator, and Consultant Thoracic Surgeon at St Vincent's Hospital Melbourne, and East Melbourne Heart and Lung, Dr Naveed Alam, exploring new treatments is critical to improving the lives of those with emphysema.
"Without proper management and treatment, emphysema can cause difficulties breathing and talking, a blue tinge to the skin due to lack of oxygen, regular chest infections and may even cause heart failure," he said.
"These symptoms can affect a patient's physical and emotional wellbeing, with up to one in three Australians living with emphysema reporting some level of disability due to the lung disease.
"Moreover, those affected are four times more likely to experience very high levels of psychological distress than those without emphysema, with breathlessness, or the fear of breathlessness, commonly causing anxiety and depression.
"Given the limited treatment options currently available to people with severe emphysema, particularly those with collateral ventilation, we hope to address this unmet need by investigating a novel treatment option through the COVE study."
What is emphysema?
Emphysema is a type of lung disease that causes breathlessness, of which there is no cure but treatments can help ease the symptoms.
With emphysema, the lungs' air sacs become damaged and destroyed, causing them to lose elasticity. As severe emphysema advances and symptoms worsen, those affected may find daily activities, such as standard exercise, hanging out the washing, food shopping, getting out of bed, and sleeping harder to do.
The disease, which develops gradually, is among Australia's leading causes of death.
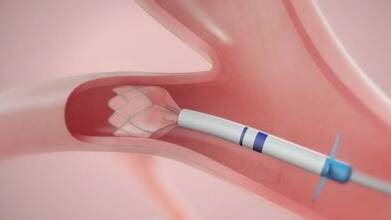
It can be treated with endobronchial valves (EBVs), valves which block air from entering the damaged part of the lung while breathing in, and allow air to escape during exhalation. They help prevent the lung from overinflating - a common symptom of severe emphysema - while still allowing trapped air to escape.
What is collateral ventilation?
This is where air flows between a lung's lobes, bypassing the normal airway. Wall-like physical dividers (also known as fissures) between a lung's lobes are not solid, allowing air to pass through one lobe to another.
People living with severe emphysema with collateral ventilation face limited treatment options due to the structure of their lungs, causing disabling symptoms and major disruption to their daily lives.
When there is collateral ventilation, EBVs struggle to successfully keep the damaged areas from re-inflating. As such, EBV treatment isn't available for people with severe emphysema and collateral ventilation.
Ok, so what's the new treatment?
The COVE study involves two treatments, spaced four weeks apart:
- Video Assisted Thoracic Surgery (VATS) fissure completion - a surgical procedure where the fissure structure in an affected lung is closed off, blocking air flow between different lobes, and
- Insertion of endobronchial valves (EBVs) - a procedure where small, one-way EBVs are into the most diseased part of the lung where the fissure was completed.
Six months after EBV insertion, the study researchers will measure each participant's lung function, lung volume, tolerance to exercise, shortness of breath, and Quality of Life (QoL) scores.
COVE study co-investigator, Director of Surgical Oncology, and Consultant Thoracic Surgeon, St Vincent's Hospital Melbourne, and East Melbourne Heart and Lung, A/Prof Gavin Wright, Melbourne, explained what this might mean for patients.
"If combining these two procedures is shown to be both safe and effective, it might eventually become an option for some people with emphysema who have previously not been suitable for surgery," he said.
Lived experience
Wife, grandmother-to-seven and COVE study participant, Cecilia, Melbourne, was diagnosed with emphysema almost 30 years ago.
"Living with severe emphysema is physically and mentally debilitating," she said.
"Not being able to breathe is terrifying. There have been times when I've been so afraid of being breathless, that I have been too scared to move. It's also demoralising being unable to look after myself."
Cecilia has chosen to participate in emphysema clinical studies to help inform additional treatment options for the disease.
"Nothing in life is guaranteed. But participating in a clinical study may help both myself, and others living with this devastating disease," she said.
How do I find out more information?
COVE study participants will be required to attend six appointments over six months, two of which will be for medical procedures, if eligible. Applicants must be willing, and able to provide informed consent. Smokers who qualify for the study will need to stop smoking for at least eight weeks before joining the study, and cease smoking after treatment.
St Vincent's Hospital Melbourne and St Vincent's Private Hospital Melbourne are now recruiting for the COVE Study. Study participants are required to travel to one of these Melbourne locations.
Patients living with severe emphysema located outside Victoria can ask their GP to refer them to one of the select hospitals in Brisbane, Sydney, Launceston and Adelaide, to help determine if they may participate in the COVE Study.
To learn more, or to register your interest in the COVE study, visit covestudy.com.au or email info@covestudy.com.au

